Pills that help you drink less or quit entirely: Antabuse, Naltrexone, and newer medications. How they work, side effects, and who benefits most.
Medication is not a cure for alcohol problems. I want to be clear about that upfront. But in my 50-plus years of clinical practice, I’ve watched the right medication at the right time make a meaningful difference for people who were privately struggling and couldn’t seem to get traction on their own. One size does not fit all when it comes to treatment, and medications are simply one more tool in a toolbox that should be tailored to the individual.
Antabuse: The Original Deterrent
Antabuse is a very old medication with a very simple modus operandi. You take a pill in the morning. It’s like swallowing an aspirin — you don’t feel anything, and it doesn’t do anything noticeable. But if you drink within about 48 hours of taking that pill, you’ll get sick. Nauseous, vomiting, the whole unpleasant experience.
The point is not to take Antabuse and then make yourself sick. The point is that knowing what will happen if you drink frees you from having to white-knuckle through every craving. It removes the option of impulsive drinking, and that breathing room can be enormously valuable in the early weeks when people are trying to establish some momentum.
Also known by its generic name disulfiram, Antabuse has been around since the 1950s. It works by blocking the enzyme that metabolizes alcohol, causing a buildup of acetaldehyde — a toxic byproduct that produces those deeply unpleasant symptoms. For people who want to stop drinking but are concerned they may not have the impulse control to get even a few days of abstinence without some kind of safety net, Antabuse can jumpstart the process.
Using Antabuse Strategically
What many people don’t realize is that Antabuse doesn’t have to be a daily commitment. It can also be used situationally. I had a patient — a successful professional in his late thirties — who had stopped drinking for several months but had a bachelor party coming up. He knew it would be a high-risk situation. So he took Antabuse the day before and sailed through the weekend without having to fight the temptation. He doesn’t take it otherwise.
This kind of strategic use is part of good relapse prevention planning. Recognizing when you’re heading into the lion’s den and having a practical tool ready — that’s clinical science, not ideology.
Naltrexone: Popular, But Limited
Then there’s naltrexone, which is probably the most talked-about medication for alcohol problems. It works by blocking opioid receptors in the brain, which reduces both the pleasurable effects of drinking and the craving to drink. It’s FDA-approved and available as a daily pill (ReVia) or a monthly injection (Vivitrol).
Here’s my honest clinical experience: naltrexone works meaningfully in less than about a third of cases. The majority of people I’ve treated don’t get significant benefit from it. That said, it’s a fairly benign medication without much in the way of side effects, so it’s often worth trying to see if you’re one of the people who responds well.
For those who do respond, naltrexone can be particularly useful for supporting moderate drinking goals or maintaining abstinence. It can help take the edge off the compulsion to keep drinking once you’ve started — it helps some people find their “off switch,” in other words.
Why Many Don’t Stay on Naltrexone
I don’t have many patients who take naltrexone for very long because they simply don’t find it particularly helpful. With newer medications showing more promising results, naltrexone is becoming less of a first choice for many clinicians, though its lower cost and broader insurance coverage still make it an accessible option.
GLP-1 Medications: A Promising Development
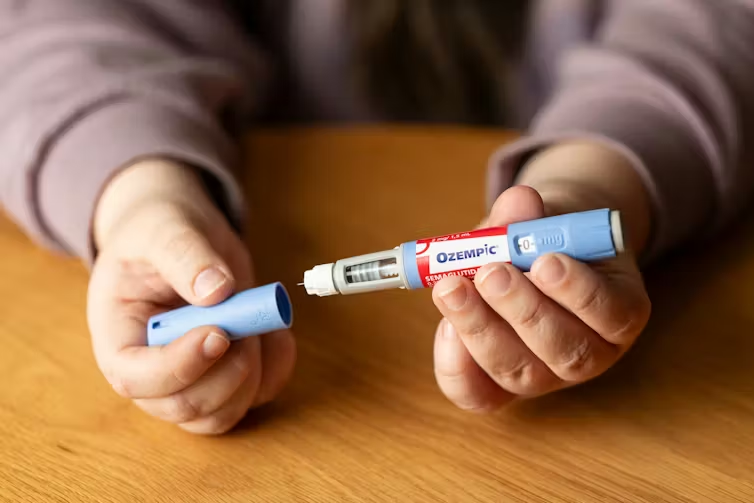
Newer medications like GLP-1 agonists — you may know them as Ozempic or Wegovy, originally developed for diabetes and weight management — have shown genuinely interesting results for reducing alcohol cravings. Research is still in the early stages, but patients taking these medications for other conditions have spontaneously reported decreased interest in drinking.
Studies suggest GLP-1 medications may affect the brain’s reward pathways in ways that dampen the desire to drink. They’re not yet FDA-approved specifically for alcohol use disorder, but the preliminary data is encouraging. The main limitation right now is cost — these medications are expensive and insurance coverage for alcohol-related use is inconsistent.
Who Should Consider Medication?
Medication as part of a structured treatment approach may be particularly worth exploring if you:
- Experience strong cravings that interfere with your efforts to cut back or stop
- Have difficulty getting through the early stages of abstinence
- Are facing high-risk situations that concern you
- Haven’t gotten the results you wanted from behavioral treatment alone
- Want additional support while working on the underlying issues driving your drinking
The key point is that medication addresses one piece of the puzzle. It can reduce cravings, create a deterrent, or take the reward out of drinking — but it rarely addresses the function and meaning of alcohol in a person’s life. That’s where therapy comes in.
Medication Works Best with Therapy
As SAMHSA’s guidance on medication-assisted treatment emphasizes, the best outcomes come from combining medication with therapy and behavioral support. In my practice, the most successful treatment plans typically involve medication to manage the biological piece, individual therapy to explore what’s driving the drinking, and often group therapy for accountability and the kind of honest feedback that only peers can provide.
Medication can open a window of opportunity. What you do with that window — the work you put into understanding your relationship with alcohol, developing better coping strategies, addressing co-occurring issues like anxiety or depression — that’s what determines long-term success.
It’s also important to be aware of potential interactions between alcohol and prescription drugs when considering any medication regimen. All medications for alcohol problems require a prescription from a licensed healthcare provider, and as NIAAA research confirms, the combination of medication and therapy consistently produces better outcomes than either approach alone.
If you’re considering whether medication might be a useful part of your treatment, a confidential conversation with a clinician who understands these options is a reasonable place to start. No pressure, no predetermined outcome — just a thoughtful discussion about what might work best for you.