A comprehensive look at FDA-approved medications that can support your recovery from alcohol problems.
Medication is not for everyone and is certainly not a cure for addiction, but it can be very helpful to a great many people. In my decades of clinical practice, I’ve seen the right medication reduce cravings, ease withdrawal, and help prevent setbacks for patients who were privately struggling with alcohol problems — whether their goal was moderation or abstinence. The mistake is thinking medication alone will solve the problem. It won’t. But as one component of a tailored treatment plan, it can make the difference between progress and stagnation.
How Medications Fit Into Treatment
Medications can also address the symptoms of co-occurring conditions — depression, anxiety, bipolar disorder — that are frequently intertwined with alcohol problems. In my experience, you rarely find one without the other. When these conditions go untreated, the person often self-medicates with alcohol, and the cycle perpetuates itself.
The question I hear often is: can someone with a drinking problem learn to drink moderately? For some people, medications that support abstinence are the answer. For others, medication may help with a harm reduction approach — helping them find their “off switch” and regain control over how much they consume. One size does not fit all.
Medication Works Best as Part of a Larger Plan
As the NIAAA treatment guide confirms, medication is most effective when combined with behavioral counseling and social supports — whether that’s participation in self-help groups or professionally-led group therapy for alcohol recovery.
While we do not prescribe medication ourselves at Recovery Options, we work closely with psychiatrists and addiction medicine specialists. This collaborative approach, built into our four-step treatment program, ensures that patients receive comprehensive care addressing both the medical and psychological dimensions of their situation.
The Medications: What’s Available and What Works
Several FDA-approved medications can help people reduce or stop drinking. For a deeper look at each option, see our complete guide to medications for alcohol problems. What works best varies considerably from person to person — which is exactly why treatment needs to be individualized.
Antabuse (Disulfiram): The Deterrent Approach
Antabuse is one of the oldest medications for alcohol problems, first approved by the FDA in 1951, and its simplicity is its strength. You take a pill in the morning — it’s like swallowing an aspirin, you don’t feel anything. But if you drink within about 48 hours, you’ll get extremely sick: nausea, vomiting, headache, chest tightness. The medication blocks the enzyme that metabolizes alcohol, causing a buildup of acetaldehyde that produces a powerful aversive reaction.
What makes Antabuse valuable is that it removes the option of impulsive drinking. You don’t have to white-knuckle through every craving or rely entirely on willpower. Knowing the consequences are certain frees you to focus on building the other skills and habits that support recovery. For people who want to stop but are concerned about impulse control in the early weeks, Antabuse can jumpstart the process — especially when paired with a clear action plan for abstinence.
I’ve also seen Antabuse used strategically, not daily. One patient took it before attending a bachelor party where heavy drinking was guaranteed. He sailed through the event without the constant internal battle over whether to have a drink. That’s practical, intelligent use of a clinical tool.
Naltrexone (ReVia, Vivitrol): Reducing the Reward
Naltrexone works differently. Rather than making you sick if you drink, it blunts alcohol’s effects by blocking opioid receptors in the brain. This reduces both the pleasure you get from drinking and the craving to drink in the first place. It’s available as a daily pill or a monthly injection — the injection being particularly useful for people who have difficulty with daily medication adherence.
Here’s my honest assessment: in my clinical experience, naltrexone produces meaningful benefit in less than about a third of cases. Many patients try it and don’t find it particularly helpful. That said, it’s a relatively safe medication with minimal side effects, so it’s often worth a trial to see if you’re among those who respond. Research shows it’s most effective at reducing binge drinking episodes and heavy drinking days, which makes it potentially useful for people working toward moderation.
If you drink while taking naltrexone, you won’t get sick the way you would on Antabuse. You’ll simply find that alcohol doesn’t deliver the same buzz or satisfaction. For some people, that reduced reward makes alcohol less appealing and easier to resist. For others, the absence of a strong deterrent means they continue drinking anyway. This is precisely why medication needs to be combined with therapy — the psychological work matters as much as the pharmacology.
According to SAMHSA, medication-assisted treatment is most effective when integrated with counseling and behavioral strategies that help you develop new ways of coping.
GLP-1 Agonists: The Promising New Development
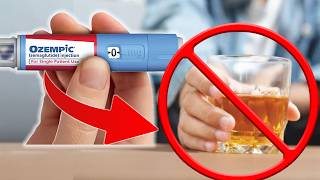
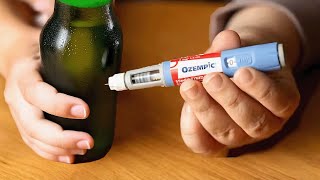
Medications like Ozempic and Mounjaro — GLP-1 receptor agonists originally developed for diabetes and weight management — are showing genuinely exciting results for reducing alcohol consumption. These medications work on brain reward pathways that affect both food and alcohol cravings, and many patients report a marked decrease in their desire to drink.
While not yet FDA-approved specifically for alcohol use disorder, preliminary research is encouraging enough that many clinicians are prescribing them off-label with impressive results. The primary limitation is cost. These medications are expensive, and insurance coverage for alcohol-related use remains inconsistent.
As research continues, GLP-1 agonists may become a front-line option. For now, they represent a window of opportunity for people who haven’t responded to traditional medications.
Other Medications Worth Knowing About
Several additional medications show promise:
- Acamprosate (Campral): Helps restore balance to brain chemistry disrupted by chronic drinking and can reduce symptoms of protracted withdrawal
- Gabapentin: Reduces cravings and anxiety in early recovery, particularly helpful for people with co-occurring anxiety
- Topiramate (Topamax): Originally an anti-seizure medication, it shows promise for reducing heavy drinking days when used off-label
The key is finding what works for your specific situation, while being mindful of dangerous interactions between alcohol and prescription drugs. This requires working with a healthcare provider who understands addiction medicine and can tailor the approach to your individual needs, goals, and medical history.
The Bottom Line
Medication addresses the biological piece of the puzzle — cravings, withdrawal, the brain’s reward response. But alcohol problems never develop in a vacuum. There are always underlying factors: stress, emotional pain, relationship difficulties, co-occurring depression or anxiety. Medication can open a window of opportunity, but what you do with that window is what determines long-term outcomes.
If you’re exploring whether medication might be a useful component of your treatment, a confidential conversation with a clinician who understands these options can help you think through what makes sense. No labels, no pressure — just a practical discussion about what tools might work best for your situation.