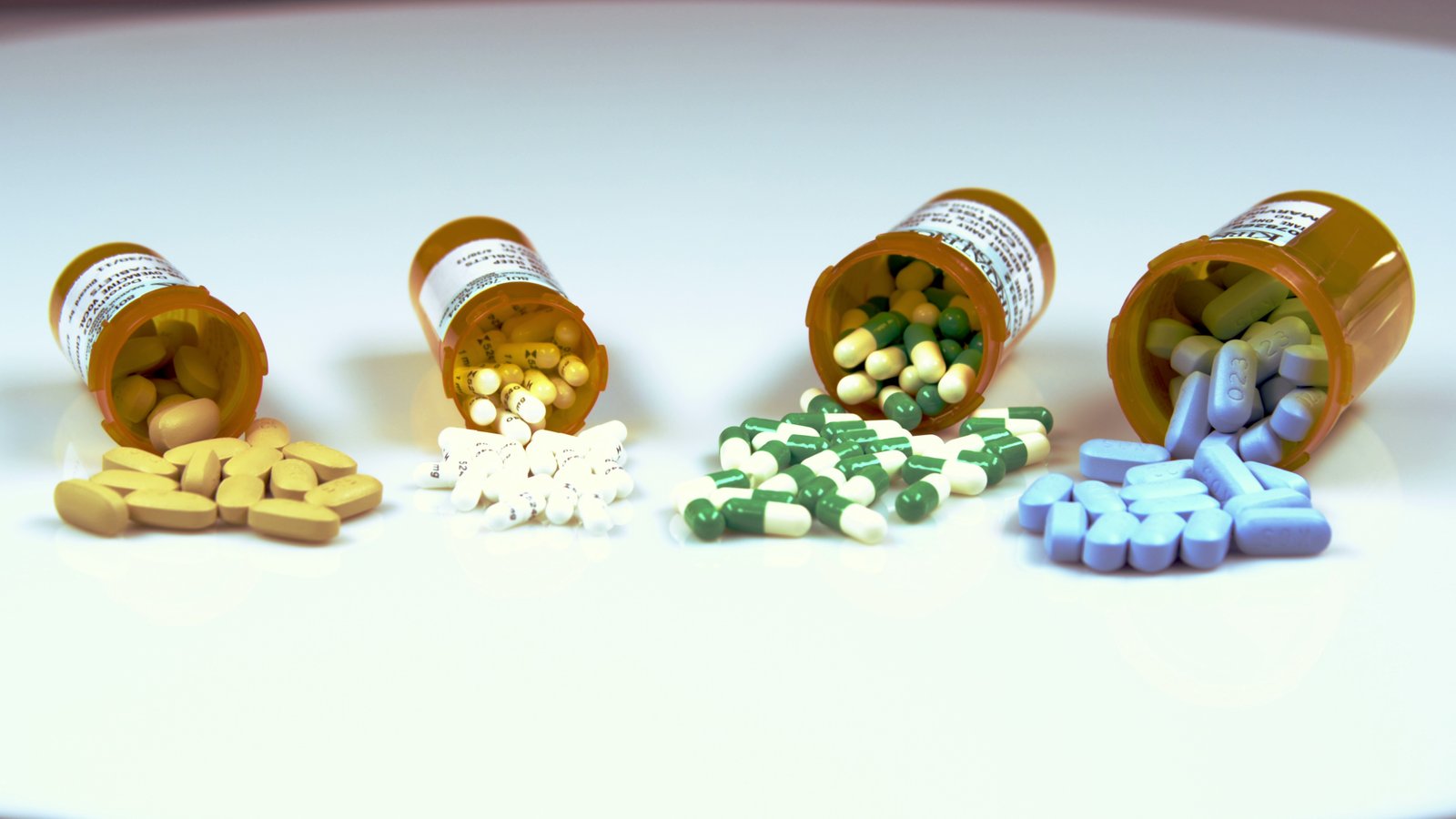
Mixing alcohol with prescription medications? The combinations that can be dangerous and how to stay safe.
Here’s something I see far too often in my practice: an intelligent, high-functioning professional who drinks moderately — or sometimes more than moderately — without giving a second thought to the prescription medications sitting in the medicine cabinet. The assumption is that if a doctor prescribed it, it must be safe. But mixing alcohol with certain medications isn’t just inadvisable. It can be lethal.
Why This Combination Is So Dangerous
Alcohol is a central nervous system depressant. It affects nearly every organ system in your body. The FDA warns that mixing alcohol with medicines can be harmful. When you add prescription medications to that picture — especially ones that also depress the central nervous system — you create interactions that can intensify the effects of either substance, create entirely new and unexpected reactions, render medications ineffective, cause liver damage, lead to respiratory depression, and increase fall risk dramatically.
This isn’t only relevant to people with severe alcohol problems. Understanding the alcohol use disorder spectrum helps clarify why even moderate drinking can become dangerous when certain medications are involved. It’s a pharmacological issue, not strictly an addiction issue.
According to the National Institute on Alcohol Abuse and Alcoholism, older adults face particularly high risk because they tend to take multiple medications and their bodies process both alcohol and drugs more slowly. If you’re over 50, our article on drinking problems later in life addresses these vulnerabilities in more detail.
How Alcohol Interacts with Medications
The mechanisms are varied, which is part of what makes this so treacherous. Additive effects occur when both alcohol and the medication depress the central nervous system, producing a combined impact far stronger than either alone. Metabolism competition happens when your liver must process both substances simultaneously, allowing toxic levels to accumulate. Alcohol can amplify side effects like drowsiness and impaired judgment, reduce a medication’s effectiveness entirely, or create toxic metabolites that damage organs.
The Most Dangerous Combinations
Opioid Pain Medications
Combining alcohol with opioid painkillers — oxycodone, hydrocodone, morphine, codeine — is among the most dangerous things a person can do. Both are central nervous system depressants, and together they can cause respiratory depression severe enough to stop breathing, loss of consciousness, overdose, and death. Many fatal overdoses involve both opioids and alcohol rather than opioids alone. Understanding how medications work in the body provides useful context here.
Benzodiazepines
Medications like Xanax, Ativan, Valium, and Klonopin should never be combined with alcohol. Even small amounts of alcohol with benzodiazepines can cause extreme sedation, respiratory depression, memory blackouts, and severely impaired motor function. This is one of the most dangerous drug combinations that exists, and I’ve seen its consequences more times than I care to count.
Sleep Medications
Prescription sleep aids — Ambien, Lunesta, Sonata — mixed with alcohol create excessive sedation, impaired judgment, and dangerous sleepwalking behaviors. I’ve had patients tell me they drink a glass or two of wine to unwind, then take a sleep medication when the wine doesn’t do the job. That’s a recipe for disaster.
Antidepressants and Mood Stabilizers
Mixing alcohol with antidepressants or mood stabilizers can worsen depression and suicidal ideation, cause dangerous blood pressure changes, trigger seizures, and reduce the medication’s therapeutic effect. For people managing co-occurring mental health conditions, alcohol can fundamentally undermine treatment. This is one reason I often recommend sobriety sampling — a period of abstinence — so patients can see how their mental health improves without alcohol in the picture. The Mayo Clinic’s overview of alcohol use disorder provides additional context on how alcohol affects mental health conditions.
Blood Thinners and Heart Medications
Alcohol interferes with blood-thinning medications like warfarin, increasing the risk of dangerous bleeding, hemorrhage, or stroke. With blood pressure medications, it can cause excessive drops leading to dizziness, fainting, and cardiovascular complications.
Who Is at Greatest Risk?
Several groups face elevated danger. Older adults metabolize both alcohol and medications more slowly. Women generally process alcohol at a different rate than men. People on multiple medications face more potential interactions. Those with liver or kidney problems have reduced capacity to clear substances from their system. And high-functioning professionals — who may be managing regular alcohol consumption alongside one or more prescriptions — often don’t realize the risk because they don’t see themselves as having a “problem.”
What You Can Do
Start by reading all medication labels and looking for warnings about alcohol interactions. Ask your doctor and pharmacist directly about every medication you take. Be honest about how much you drink — your healthcare providers need accurate information to keep you safe.
If you take medications that interact dangerously with alcohol, reducing or stopping your drinking becomes a medical priority, not just a lifestyle choice. If cutting back proves difficult, there are medications that can help with alcohol problems — an option worth exploring with a professional who understands both sides of the equation.
The goal here isn’t to create alarm. It’s to give you the information you need to make intelligent decisions about your health. If you’re concerned about how your drinking interacts with your medications, a confidential consultation can help you sort through your options and find a path that makes sense for your situation.